 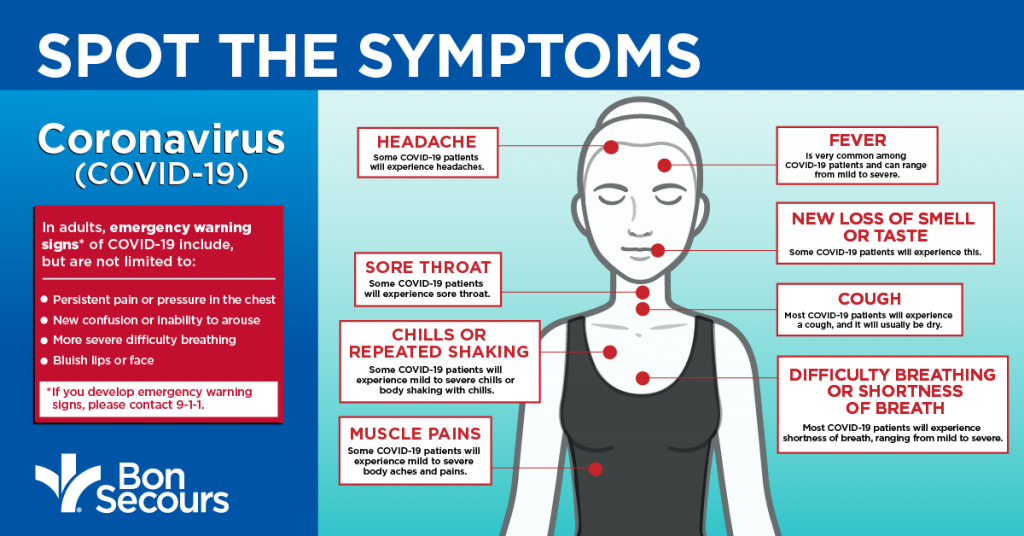
But a few other strains are beginning to cause an increasingly large share of cases. This omicron subvariant is still in the lead and now responsible for just about 30% of COVID-19 cases, CDC data show. Or it might just be a sign that the virus has found its optimal form - for now.īack in late August, BA.5 hit its peak and accounted for nearly 85% of all COVID-19 infections in the U.S. Having a group of emerging omicron-related variants rather than one clearly dominant strain may signal a shift in the pandemic, experts told TODAY. The current landscape of COVID-19 variants “Someone that’s fully vaccinated and up to date may have such mild symptoms that they don’t even test themselves,” Yang said. The protection gained from vaccination and previous infections could also have reduced the overall severity of symptoms over time, the experts noted. according to CDC data, they comprise about 3.4% of cases.Įven as scientists investigate the current, most common COVID symptoms, it can be challenging to truly track changes in symptoms over time, Yang said, because so many fewer positive cases are officially recorded now. It's worth noting, though, that BA.2 and its descendants haven't been prevalent in the U.S. About 82% of respondents had fever, followed by just under half having a cough. “And that’s probably related to why it’s less deadly: It’s not affecting the lungs as much.” So doctors are seeing more things like sore throat and runny nose than they did with previous versions of the virus, he said.Īnother recent study published in medical journal Cureus found fever to be the most common symptom among a group of 228 people in India infected with variants descending from BA.2. Otto Yang, professor of medicine in the division of infectious diseases and of microbiology, immunology and molecular genetics at the David Geffen School of Medicine at UCLA, told TODAY. “The general impression among clinicians is that omicron tends to stay more in the upper respiratory tract,” Dr. Meanwhile, some of the symptoms that were previously considered classic signs of COVID-19 - loss of taste or smell, fever, shortness of breath - are not ranking as highly anymore, a report from the company says. "This trajectory (is going) really high, and we don’t know what’s going to happen." John Torres, NBC News senior medical correspondent, in a Nov. 
"These things typically don’t peak until the December to February timeframe, and we’re not in December yet,” said Dr. 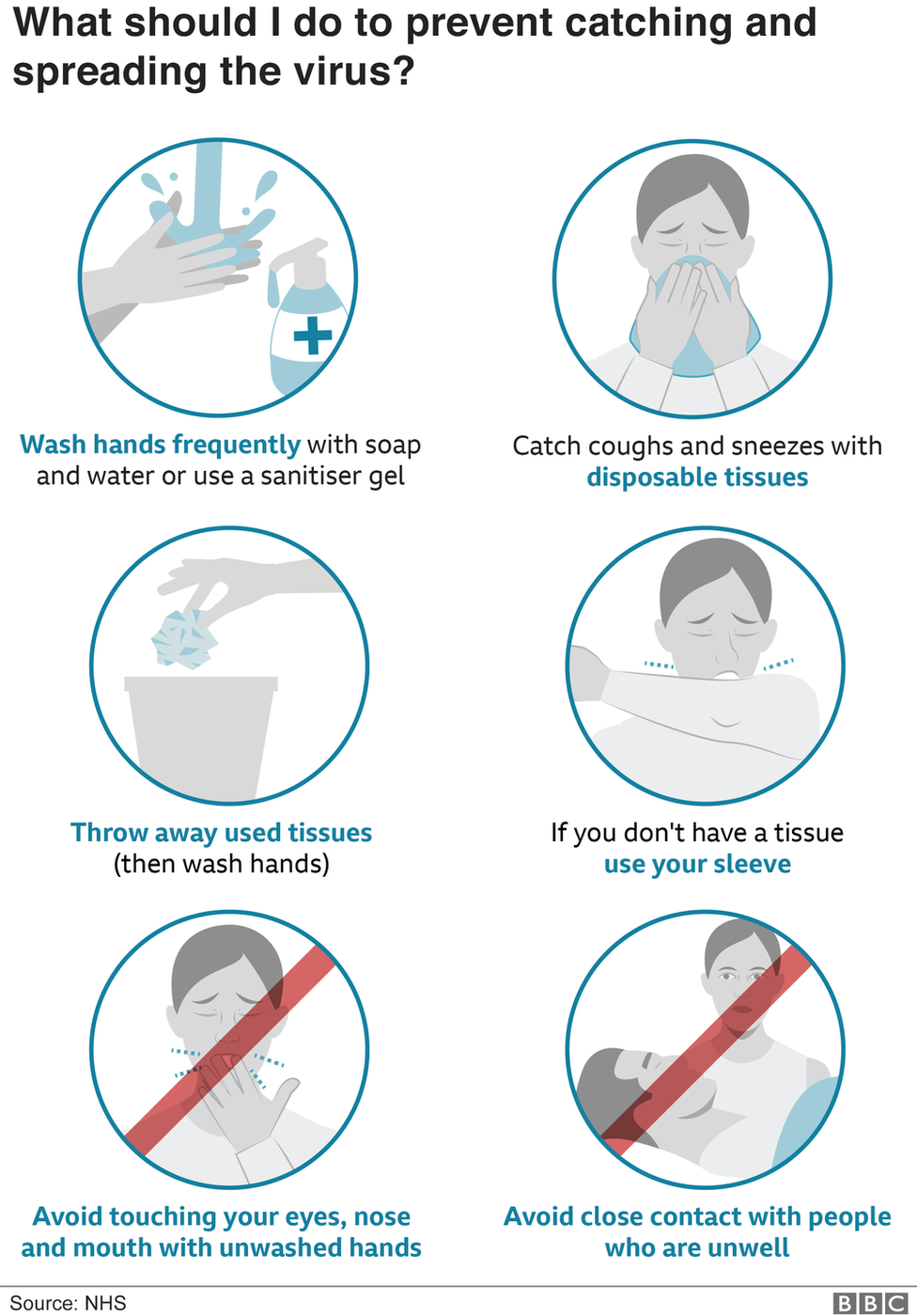
The possibility of respiratory illnesses like RSV and influenza continuing to spread at the same time as a potential COVID-19 wave is being referred to as a "tripledemic." Experts are fearing this could occur because cases of RSV (a common childhood virus) and flu are already sending so many people, including kids, to hospitals. health care system, there's also merit to wearing masks in crowded, indoor spaces, TODAY previously reported. And given the current surges of RSV and flu, which are straining the U.S. Whatever happens, there's still no harm in taking a COVID test before a holiday gathering, especially if you've recently spent time with a large group of people inside, or if someone high risk for severe illness will be at the gathering, experts previously told TODAY. I’m pretty much living life the way I was living life in 2019.” "We are now at a point where I believe if you’re up to date on your vaccines, you have access to treatments … there really should be no restrictions on people’s activities. 14 meeting of health officials, Stat News reported. "We are in a very different place and we will remain in a different place,” Jha said during a Nov. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
